Tourette syndrome is a type of tic disorder. Awareness of Tourette’s statistics can help those impacted find appropriate care and treatment.
There are many misconceptions aboutTourette syndrome (TS), often spread by its portrayal in the media. For example, many people think that Tourette’s involves swearing uncontrollably, but that only happens in a small number of people with the condition.
In reality, Tourette’s is a neurological condition that affects the brain. Usually, it starts in childhood or teenage years. Its characteristic trait is muscular or vocal tics, which are uncontrollable, sudden movements or sounds. Frequently, people with Tourette’s also have other medical or behavioral conditions.
Here, we present somefacts and statistics about Tourette Syndrome. With greater awareness, people with Tourette’s and those who know them can understand the condition better and find help easier.
How Common Is Tourette Syndrome (TS)?
Since many people with Tourette’s are not diagnosed correctly, it is hard to say exactlyhow common Tourette Syndrome is. One estimate says that about0.6%of children, or 1 in every 162 kids, has Tourette’s. A study conducted by the Centers for Disease Control and Prevention found that 1 in 360 kids, or about0.3%of children, had a diagnosis of Tourette’s, meaning that only abouthalfofchildren with Tourette’sare diagnosed.
Theprevalence of Tourette Syndromeis much higher in boys than in girls. Boys are3 to 4 timesas likely to have Tourette’s as girls. Adolescents 12 years or older aretwice as likelyto be diagnosed with Tourette’s as children aged 6 to 11. Tourette’s is more common innon-Hispanic whitechildren than children of other ethnicities.
Diagnosing Tourette’s
There are no specialized tests to diagnose Tourette Syndrome. Usually,Tourette’s is diagnosedby a family doctor during a routine checkup. During this checkup, the doctor will ask questions to determine what kind of tics a child has, how often they occur and how long the child has had them.
Like other neurological conditions, Tourette syndrome is diagnosed according to guidelines established by the American Psychiatric Association. These guidelines are listed in theDiagnostic and Statistical Manual of Mental Disorders(DSM-5).
Diagnosticcriteria for Tourette Syndromeinclude:
- Multiple motor tics and one or more vocal tics (not necessarily at the same time)
- Tics have lasted for more than one year (though they can increase and decrease in frequency)
- Tics started before the age of 18
- Tics are not caused by a drug or other medical condition
Tics can start asearly as age 4, but a diagnosis can only be made after the child has had tics for at least one year.
Course of Tourette Syndrome
Fortunately, most children eventually outgrow Tourette’s, and tics rarely last into adulthood. Usually, tics start appearing between ages5–7and peak around age8–12. By early adulthood, the severity of tics is significantly reduced in aboutthree-quartersof people with Tourette’s, whileover one-thirdare completely tic-free. SinceTourette’s usually doesn’t last longinto adulthood, itsprognosisis favorable.
Rates of Tourette’s and Co-Occurring Conditions
Other medical conditions, especially other neurological disorders, are common among people with Tourette’s. Of children diagnosed with Tourette’s,86%are diagnosed with other behavioral,mental health, or developmental disorders.
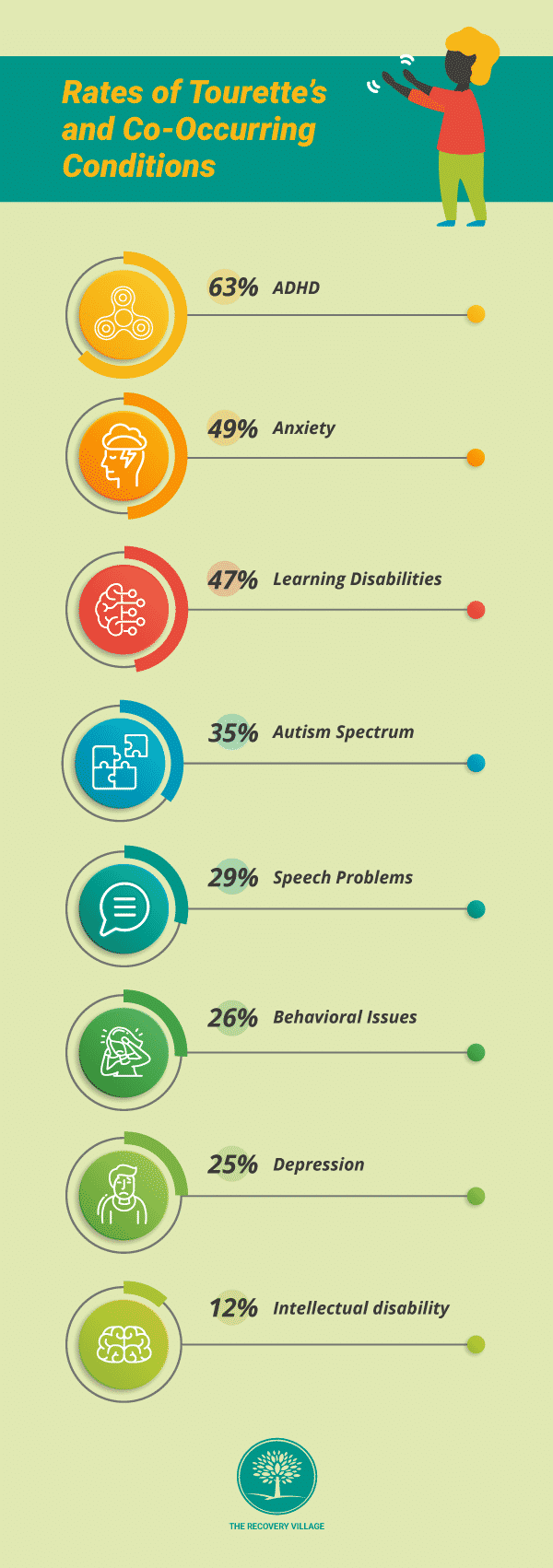
Theratesof common co-occurring conditions among Tourette’s patients vary:
- Attention-deficit hyperactivity disorder(ADHD): 63%
- Anxiety: 49%
- Learning disabilities: 47%
- Autismspectrum disorder: 35%
- Speech or language problems: 29%
- Behavioral or conduct issues: 26%
- Depression: 25%
- Intellectual disability: 12%
Public Health Impact of Tourette’s
Tourette’s can require significanthealthcare costsfor patients with the condition. Costs can come from:
- Doctor appointments
- Medications
- Counseling or therapy sessions
- Educational accommodations
The long-term impact of Tourette’s on a child’s mental and physical health andeducationcan also have negative effects on their employment, social life and family relationships.
The fullpublic health impactof Tourette’s is not fully understood. Fortunately, as publicawareness of Tourette Syndromeincreases, medical professionals learn more about the condition and the best ways to manage it.
Statistics on Tourette’s Treatment
Tics are usually mild, andthe vast majorityof Tourette’s cases do not need to be treated medically. However, tics should be addressed if they are interfering with a person’s daily life.Treatment for Tourette’smayinvolve medicationto control impulsive behaviors, along with counseling and physical or occupational therapy. Theoutcome of this treatmentis usually a reduction in the frequency or severity of tics. However, Tourette’s cannot be cured, and tics typically do not go away entirely with treatment.
Early Treatment Outcomes
Rather than medical treatment, Tourette’s is usually managed with educational interventions. About half of children with Tourette’s have an individual education plan (IEP) at their school to help with learning challenges. As of today, not much is known of the full impact ofearly interventionfor Tourette Syndrome. However,early treatmentdoes seem to improve the learning, behavioral and emotional effects of the disease.
If you or someone you love is affected by Tourette Syndrome and substance abuse, pleasecontact us at The Recovery Village. We offer comprehensive treatment for addiction and co-occurring mental health conditions at reputable centers across the country.