Statistics show that the effects of insomnia may be more far-reaching than most people think.
People may think they have a thorough understanding ofwhat insomnia isand the impact it has on the lives of those with the condition, but there may be more to insomnia than many people realize. Insomnia facts and statistics can shed new light on the condition and improve the future ofinsomnia treatment.
How Common Is Insomnia?
As far as health complications go, insomnia is relatively prevalent. The condition currently affects millions of people every year. According to theAmerican Sleep Association:
- Nearly 70 million Americans have asleep disorder
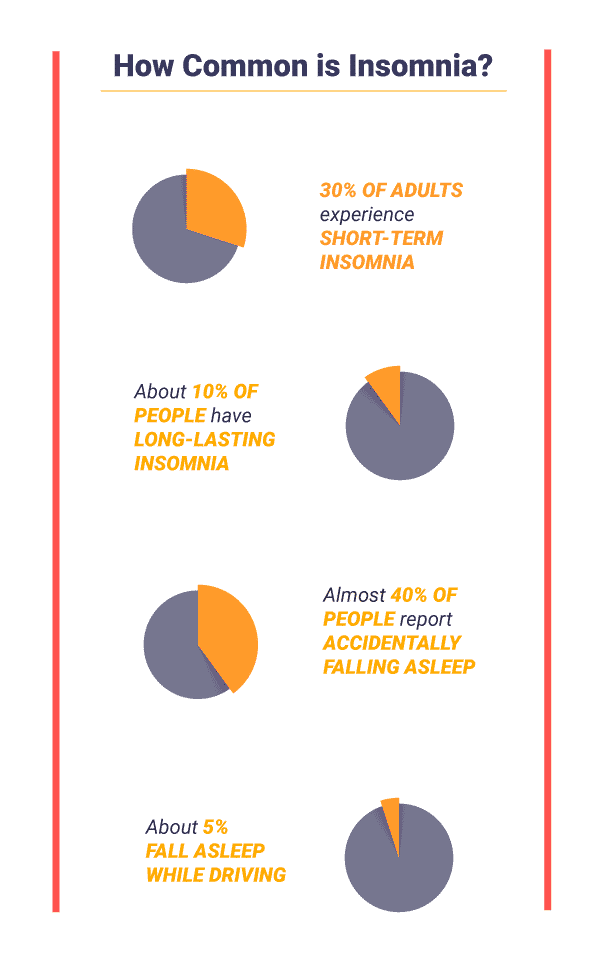
- Insomnia is the most common sleep disorder, with 30% of adults experiencing short-term insomnia
- About 10% of people have long-lasting insomnia
- Almost 40% of people report accidentally falling asleep during the day
- About 5% report falling asleep while driving
Even though adults need at least seven hours of sleep per night, about 35% of people get less than that. Age appears to be linked to lack of sleep, with 37% of people age 20–39 reporting low sleep duration and 40% of people age 40–59 getting too little sleep.
These insomnia prevalence rates are shocking considering the toll insomnia can take on mental and physical health. While the condition may seem benign, insomnia can have a dramatic effect on people’s daytime lives and even lead to death from accidents and decreased judgment.
Diagnosing Insomnia
Someone who has chronic poor sleep or problematic sleep habits should seriously consider talking to a medical professional about their situation. A properinsomnia diagnosiscan help someone receive the services they need to improve their sleep quality and overall health.
An accurate diagnosis of insomnia is especially important because, in many cases, the condition has physical andmental healthorigins. Insomnia is currently classified as a sleep-wake disorder by the American Psychiatric Association in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5).
According to the DSM-5, the criteria for insomnia disorder include:
- Intense dissatisfaction with the quality or amount of sleep caused by trouble falling asleep, difficulty staying asleep and waking up too early in the morning without being able to fall back asleep
- Sleep issues create a significant amount ofstressthat begins to impact aspects of daily life
- Sleep problems occur at least three nights each week and persist for at least three months
- Poor sleep occurs even when there is enough time devoted to sleep and rest
To gather information about a person’s sleep patterns, a medical professional will ask questions about:
- Medications used
- Caffeine, tobacco andalcoholintake
- Life stress and physical pain
- What time they go to bed and wake up
- How long they sleep for
- How well they sleep
- Snoring and breathing during sleep
One type of insomnia, called primary insomnia, lasts for a month or more and is related to external stressors in the person’s life. The causes of primary insomnia include:
- Major life changes, like moving
- High stress
- Travel or work changes
- Bad habits, like napping or going to bed too early or late
A secondary insomnia diagnosis is made when another condition causes sleep issues. A variety of problems can lead to secondary insomnia, including:
- Mental health issues
- Pain conditions
- Heartburn
- Restless leg syndrome
- Sleep apnea
- Asthma
- Menopause
Because there are many factors involved in diagnosing insomnia, open and honest communication with the medical provider is essential to receiving an accurate diagnosis and effective treatment.
Rates of Insomnia and Co-Occurring Conditions
As mentioned, insomnia and co-occurring mental health or physical health complications are relatively common. According to theAmerican Academy of Sleep Medicine:
- Stress can result inadjustment insomnia, which may affect up to 20% of people each year
- Poor sleeping habits in children can lead tobehavioral insomnia of childhood, affecting 30% of children
- Prescription drugs,substance abuse, medical disorders, and mental health conditions can cause insomnia, with about 3% of the population having this type of sleep issue. Specific causes includedepression,drug withdrawal, obesity and anemia
- A person with high anxiety and worry could havepsychophysiological insomnia, a condition affecting about 2% of the population and about 15% of sleep center patients
Insomnia and Pregnancy
Pregnancy is another condition that may result in temporary insomnia. Nearly 4 in 5 pregnant women will experience some level ofinsomnia during pregnancy. Pregnancy triggers a number of changes known to result in insomnia, like:
- Abdominal discomfort
- Back pain
- Heartburn
- Frequent urges to urinate
- Highanxiety, worry, and stress
- Hormonal changes
- Vivid dreams
Cost of Insomnia
Insomnia takes a heavy toll in the workplace. According to theAmerican Academy of Sleep Medicine, insomnia costs:
- 11.3 days of work for the average worker every year
- $2,280 in lost productivity for the average worker each year
- A total of $63.2 billion for the entire nation in lost productivity per year
Treatments can be expensive as well. The cost of filling a generic sleeping pill prescription may run $200 per year, while a course of psychotherapy for insomnia can cost up to $1,200.
TheAmerican Sleep Associationnotes the human cost of insomnia is steep, with about 1,600 deaths and 40,000 injuries caused by drowsy driving each year. Additionally, a significant portion of the 100,000 hospital deaths caused by medical errors each year can be attributed to sleep deprivation.
Statistics on Insomnia Treatment
Though insomnia can cause a heavy burden, one must remember that treatment is available and effective. Someeffective treatmentsfor insomnia include:
Regardless of the treatments used, insomnia generally improves with professional treatment. Of those with insomnia, about75%recover without their sleep problems persisting. Only about 6% of people with insomnia go on to develop chronic insomnia symptoms.
Insomnia Prognosis and Outlook
Overall, the prognosis and outlook for insomnia are favorable. However, it’s essential to keep in mind some risk factors associated with a poorer prognosis, including:
- High anxiety, worry and tendency to repress feelings
- Being an older woman
- Family members with insomnia
- Poor sleeping conditions
- Excessive caffeine use
- Drug and alcohol use
- Irregular sleep schedules
If you or someone you care about is affected byco-occurring insomnia and substance use disorder, calling The Recovery Village can start the treatment process. When you speak to a representative from The Recovery Village, they can offer available treatment options for someone with insomnia and substance use issues.Reach outtoday for more information.















