The following provides an overview of heroin, intravenous drug use, and what the term “heroin arm” refers to.
Heroinis a dangerous, addictive and often deadly opioid. When people take heroin, it affects their brain and essential functions including respiration.
During the 1970s, the use of heroin was almost strictly associated with intravenous drug use. While that trend has changed with more people nowsmokingorsnortingit, injecting heroin is the most common way people take heroin.
The following information provides an overview of heroin, intravenous drug use, and what the term “heroin arm” refers to.
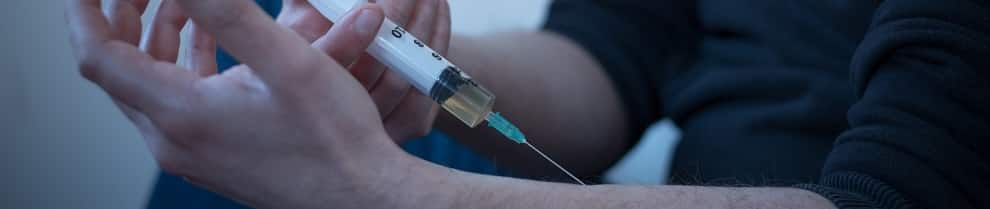
What is Heroin Arm?
Heroin is an illicit drug sold on the streets that’s a large part of the opioid epidemic in the United States. Countlessoverdoseand deaths occur because of heroin as it continues to spread in many communities.
When someone takes heroin, it binds to opioid receptors in their central nervous system and this triggers a flood of dopamine that’s responsible for the euphorichighand pleasurable feelings people say they have when they use this drug. In the process, heroin also activates the brain’s reward pathways. When this occurs, the brain wants to keep seeking out what provided that pleasurable feeling. Unfortunately, because what the brain seeks is heroin, this is when addiction develops. People also become tolerant of heroin meaning they need higher doses to have an effect, and if they try to stop using heroin they can experiencewithdrawal symptoms.
Along with feeling high, heroin use also causes people to feel very drowsy and even nod off. Heroin has many other adverseside effectslike nausea, vomiting and itchiness. Of course, overdosing is possible and frequently happens with heroin use. Signs of a heroin overdose include slow, shallow or erratic breathing, along with unconsciousness, cold, clammy skin and having a bluish tint to the lips and pinpoint pupils.
“Heroin arm” is a term that refers to the scarring that happens when someone injects the drug repetitively over time. Increasingly pure products have allowed people to take heroin in other ways aside from injecting it with a needle, but even if someone ultimately starts out snorting or smoking heroin, they tend to shift to injecting it, which leads to heroin arm.
The reason for this trend toward injecting is because when heroin is injected it works quickly and people often feel the effects within a few seconds. Injecting heroin also causes a stronger high than the alternative methods provide.
Unfortunately, there are also additional risks that come with injecting heroin, in addition to the risks of the drug itself.
Heroin Marks on the Arm
Heroin marks on the arm can be one of the tell-tale signs that someone is using the drug. Many people who use drugs become adept at hiding these marks, which are also called “track marks.” They may inject heroin in places other than their arm, for example, or they may wear long sleeves year-round.
There are many dangers associated withinjecting heroin. First, the risk of overdose is higher when someone injects the drug. Also, if someone is using heroin that’s cut with toxins or has other additives they’re unaware of, it can be even more dangerous to put the drug directly into the bloodstream.
There are also the risks associated with needle use including the heightened risk of contracting diseases like HIV and hepatitis. Also, when people have visible heroin marks on their arm, it can mean they’re at a higher risk of complications like inflamed or collapsed veins, skin infections or other problems.
Heroin Arm Infection
A heroin arm infection is a common complication of intravenous use of the drug. There are different types of heroin arm infections that can occur as well.
People can get a bacterial heroin arm infection when they have germs that are on their skin’s surface or on aneedle. Via injection, they push the bacteria deep into their skin and bypass the skin’s protective layer. If a bacterial heroin arm infection reaches blood vessels, it can cause very deep infections in the tissues, veins or vascular areas. People who inject heroin subcutaneously are at risk of getting abscesses and infected blisters.
Staph infections are associated with injecting heroin and intravenous drug use, and these infections can start out looking like a pimple or bug bite. They may appear swollen, sore and red. Staph infections can spread to other areas of the body and require intravenous antibiotics and drainage of the wound area. Abscesses are infections that lead to a mass that’s filled with bacteria, debris, and pus.
Cellulitis is a skin infection that leads to streaking of the skin, swollen lymph nodes, leaking yellow fluid from blisters and fever. Sometimes cellulitis requires hospitalization.
Necrotizing fasciitis is a flesh-eating disease that occurs when bacteria enters the tissue. Skin starts to feel swollen and hot and people also often have symptoms like fever, vomiting, and diarrhea. Skin can blacken as the infection spreads and it can lead to death if it spreads far enough. Amputation may also be necessary in some cases.
Heroin marks on the arm are indicators that someone is repeatedly injecting drugs into their arm, creating the scars. Heroin arm is a key sign of drug use in many people.
If you or someone you know is using heroin, help is available.Call The Recovery Villagetoday to learn abouttreatmentoptions and begin the journey to long-term recovery.













