Fentanyl is finding its way into many street drugs and driving the increase in drug overdose fatalities. Withdrawal and detox are the first steps to overcoming fentanyl addiction.
The first step of recovering fromfentanyl addictionis ridding the body of fentanyl and its toxic metabolites. This process is known asdetoxificationor detox. As the body clears the fentanyl and adjusts to its absence, the unpleasant experience of withdrawal occurs.
Many people who use substances want to escape their addiction, but fear of withdrawal keeps them from trying. However, millions ofpeople have found long-term recovery, and that period of detox and was a small but necessary price to pay for huge rewards.
Fortunately, withdrawal and detox symptoms can be managed in a medical setting. By participating in an inpatient detox and withdrawal program, people can get through the experience safely and more comfortably.
What is Fentanyl Withdrawal?
Doctors prescribe fentanyl to sedate patients briefly during painful procedures, such as fixing a dislocated shoulder or straightening a broken bone, or for end-of-life pain management for terminal patients. Fentanyl is extremely potent, so doctors can prescribe a tiny dose. It has a very quick onset of action and is quickly eliminated from the body.
These same properties — high potency, quick onset of action and short half-life — make fentanyl ideal for drug dealers. Tiny amounts of the powder can be put into drugs to increase potency, create “fake” drugs or make it easier to smuggle. People get high very quickly, and then the drug is rapidly metabolized by the body. This makes withdrawal symptoms appear quickly, and people who use fentanyl are compelled to go out and pick up another dose very soon.
Many people are addicted to fentanyl without even realizing it. Some illicit drug dealers make fake heroin with it, and many people treated for “heroin overdose” have no actual heroin in their system. The drug they thought was heroin was simply fentanyl and cutting agents. Even cocaine — a non-opioid — is being faked with fentanyl, which has led to an increase in fentanyl overdose cases. Synthetic opioids like fentanyl and its related compounds are currently the main drivers of drug overdose deaths in the U.S. This makes recovery from drug use more urgent than ever before.
Fentanyl Withdrawal Symptoms
When a person uses opioids, their body gradually acclimates to the presence of the drug. When the drug is no longer regularly used, the person experiences withdrawal symptoms as their body copes with the absence of the substance.
Symptoms of fentanyl withdrawal can include:
- Sweating
- Chills, fever or goosebumps
- Exhaustion
- Cognitive problems
- Anxiety
- Restlessness
- Insomnia
- Aches and pain
- Abdominal cramps
- Gastrointestinal problems including diarrhea, nausea or vomiting
People going through withdrawal often experience what can feel like depression because of how the opioid impacts their dopamine and neurotransmitters, which are responsible for how their brain experiences pleasure. This can last longer than many of the other side effects of withdrawal.
Fentanyl Withdrawal Timeline
Because of fentanyl’s short half-life, withdrawal symptoms usually begin within 12 hours of the last use. This can be longer in people who were using the fentanyl patch, which is a slow-release delivery system that releases the drug over 72 hours. In that case, withdrawal symptoms usually start after the patch is removed.
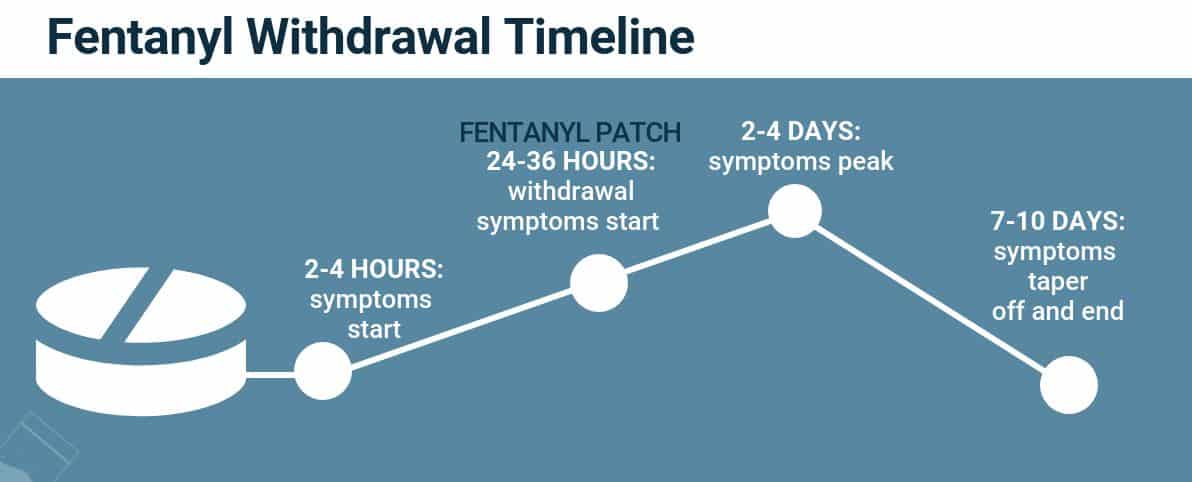
Stages of Fentanyl Withdrawal
Withdrawal symptoms from fentanyl can vary in severity at different stages after discontinuing use. The duration of fentanyl withdrawal can be broken down into three stages:
Early:
Withdrawal symptoms from opioids usually begin around 12 hours after the last dose is taken.
Peak:
The peak effects of withdrawal are often seen anywhere from one to two days after the last dose of fentanyl.
Long-Term:
Within about three to five days, most of the symptoms come to an end. However, people can experience emotional issues after they stop using fentanyl. These are often called post-acute withdrawal symptoms, and they may occur for a few months after stopping fentanyl.
Typical psychological symptoms that occur during post-acute withdrawal include:
- Anhedonia (inability to experience pleasure)
- The “pink cloud” syndrome (excessively happy feelings, ignoring the reality of life)
- Negative feelings typical of addiction, such as guilt, remorse, self-loathing, low self-esteem and anger

These symptoms are an especially potent cause of relapse. Because of them, proper rehab treatment is necessary to help people return to good mental and physical health and maintain lasting recovery from substance use.
How Long Does Fentanyl Withdrawal Last
Fentanyl’s withdrawal timeline and duration are variable. It depends on several factors, including:
- The individual’s state of physical and mental health
- The genetic and biological characteristics of the individual
- The duration and intensity of the drug use
- Whether or not withdrawal was medically assisted
For most people, withdrawal symptomstaperoff and end after 7-10 days.
Fentanyl Withdrawal Medications
There are currently three medications approved by the FDA for use intreating opioid withdrawal:
- Methadone: opioid replacement
- Buprenorphine: opioid replacement
- Extended-releasenaltrexone: blocks opioid effects
With opioid replacement therapy, a long-acting opioid medication such as methadone or buprenorphine is used to keep drug cravings and withdrawal symptoms to a minimum. The dose of these drugs is then tapered in a slow and controlled manner until the recipient is opioid-free.
Of the two FDA-approved opioids for the treatment of fentanyl withdrawal, buprenorphine generally has a more favorable side-effect profile than methadone. The buprenorphine product Suboxone is commonly used during opioid detox. Besides buprenorphine, Suboxone also contains naloxone, which blocks opioid receptor sites to prevent any attempts of abuse.
Related Topics:
Same day suboxone treatment
Suboxone addiction treatment near me
Extended-release naltrexone is a non-opioid medication, but it reduces cravings by blocking opioid receptors in the brain. If the recipient relapses and uses opioids, the naltrexone will block the physical effects of the drug. Unfortunately, the recipient must already be detoxed from fentanyl before starting this medication. Otherwise, it will worsen the withdrawal symptoms.
Other medications may also be used during fentanyl detox in order to help with specific symptoms. These include sedatives, such as benzodiazepines, and the medication clonidine, which helps reduce some withdrawal symptoms.
Fentanyl Withdrawal Deaths
Despite the toxic lethality of fentanyl, withdrawing from fentanyl use is safer than withdrawing from alcohol. Opiate withdrawal, however, is occasionally fatal. When people die from fentanyl withdrawal, it’s usually due to vomiting and diarrhea, which are typical withdrawal symptoms. If left untreated, these symptoms can rapidly dehydrate the body and cause dangerously high levels of sodium to accumulate in the blood (hypernatremia). This can cause the heart to fail.
These cases occur when people withdraw from fentanyl on their own, usually in a jail setting. Such deaths can be prevented by medical supervision in a detox facility.
Fentanyl Withdrawal Cold Turkey
Stopping fentanyl “cold turkey” results in a rapid onset of withdrawal symptoms that are usually severe. The risk of relapse during withdrawal is high, as the craving to use fentanyl to stop the symptoms can be overwhelming. When people try to self-taper their fentanyl, they are rarely successful because the ability to control substance use is not in the nature of addiction.
Quitting cold turkey is not recommended, as it is the most difficult way to stop fentanyl use. Rather, medically supervised detox, medications, fentanyl abuse counseling support and symptom management make the experience much easier, safer and more likely to result in a successful recovery.
Weaning Off Fentanyl
Weaning or tapering off fentanyl can be beneficial. It may extend the overall period of withdrawal, but it reduces the severity of the withdrawal symptoms a person may experience. Tapering off fentanyl should be done in a medically supervised environment, where a physician will create a plan to slowly lower doses of fentanyl until a person can stop safely.
Weaning can also help alleviate some of the risks of withdrawal from fentanyl, such as aspiration, dehydration and relapse.
Fentanyl Withdrawal Tips
The biggest tip for heroin withdrawal is to not do it alone. Withdrawal is usually a cruel ordeal, and thewillpower to overcome addiction is rarely enoughto make it through. There is excellent professional help available to make withdrawal safe, comfortable and provide a foundation for long-term recovery. Aspecialized treatment facilitywith medically assisted detox is the safest method for quitting fentanyl use and avoiding relapse.
Fentanyl Detox
Fentanyl detox involves the medically supervised withdrawal from fentanyl, which helps provide optimal safety and comfort. Detox should be done as part of an overall plan for recovery. It is important to keep in mind that recovery from substance addiction takes much more than simply ending drug use. The underlying causes of the addiction and the mental devastation from the addiction itself must be addressed for the best chances of a successful recovery.

Medical Detox from Fentanyl
Medical detox involves the use of medications and medical supervision to safely withdraw from fentanyl or other substance use. An inpatient detox program forms the first part of a substance addiction treatment program and is a natural transition to counseling, which forms a crucial part of the overall treatment plan.
Can You Detox From Fentanyl at Home?
When deaths have occurred from fentanyl withdrawal, they have almost always been in people who were alone at the time. Because of fentanyl’s ultra-high potency and its short half-life, withdrawal from thisopioidcan be especially harsh, and people who try to detox on their own might not succeed. They are putting themselves through unnecessarily difficult symptoms.
People considering detoxing from fentanyl at home should do so under the care of their doctor. They should also be honest with their doctor about their drug use so they can receive the appropriate advice and care.
The internet is brimming with various chemicals and remedies that are promised as a way to detox from fentanyl, but caution is advised. Most are unproven, untested and unregulated. It is advisable to speak with a healthcare professional before taking any such medicines.
There are some over-the-counter medications that can help with some of the withdrawal symptoms, such as antidiarrheals and antinauseants to help with stomach symptoms and acetaminophen for muscle aches.
People who plan to detox at home should have some characteristics in place:
- They have not been addicted to fentanyl for long
- They should have a stable and supportive home environment
- They should not live alone, and the people at home should be aware of the detox situation
- They should be highly motivated to recover
Remember that detox does not in any way constitute treatment for fentanyl addiction. People should find treatment to address the reasons behind the substance use and recover from the mental and physical damage caused by drug use.
Helping Someone Withdrawing or Detoxing From Fentanyl
Before helping a loved one through the withdrawal process, it is best to talk to a medical professional who is familiar with fentanyl addiction detox.
People with an addiction often overestimate their ability to end substance use on their own, even if they have failed on multiple previous attempts. Fentanyl can be especially difficult to withdraw from. As such, it may be wise to challenge a loved one’s decision to self-detox.
It can be very stressful to watch a loved one withdraw from fentanyl. Within hours of last using fentanyl, individuals become very sick and may not appear to be themselves. Besides the physical symptoms, they may have significant outward psychological symptoms, such as confusion, anxiety and even aggression. They may beg and rationalize reasons to go out and get their drug.
Recovery is a lifelong process, and people in recovery from substance use require ongoing support. Friends and family can become involved in the recovery counseling process as well.
Finding a Fentanyl Withdrawal and Detox Center
Addiction to fentanyl is a highly damaging and potentially fatal condition, and recovering from such addiction is an urgent issue. Undergoing detox at an accredited facility is the safest and most effective way to rid the body of drugs like fentanyl and transition into treatment and recovery.
At The Recovery Village, our team of doctors and addiction professionals aim to help individuals feel as comfortable as possible during substance withdrawal. If you wish to discuss fentanyl addiction in yourself or a loved one,contact us for a confidential discussionwith one of our representatives.
Related Topic:Signs of drug use













