When people want to have an understanding of what opioid drugs are they will often compare one to another. For example, people commonly ask “Arefentanylandoxycodonethe same?” The technical answer is no, but the two drugs do have some similarities and differences.
What Are Opioids?
The primary similarity between fentanyl and oxycodone is the fact that they’re both classified as opioids.Opioidsare a class of drugs that has gained national attention in recent years because of how often they are abused.
All drugs classified as opioids have structural similarities, including fentanyl and oxycodone. Both of these substances interact with opioid receptors found throughout the body and the brain. While prescription opioids including fentanyl and oxycodone are designed to treat pain, they can also create a euphoric high, particularly when taken in larger doses. This euphoric high is why opioid use involves a significant risk of abuse or addiction.
Fentanyl and oxycodone are both synthetic opiates, meaning they are made in a laboratory, rather than being naturally occurring.
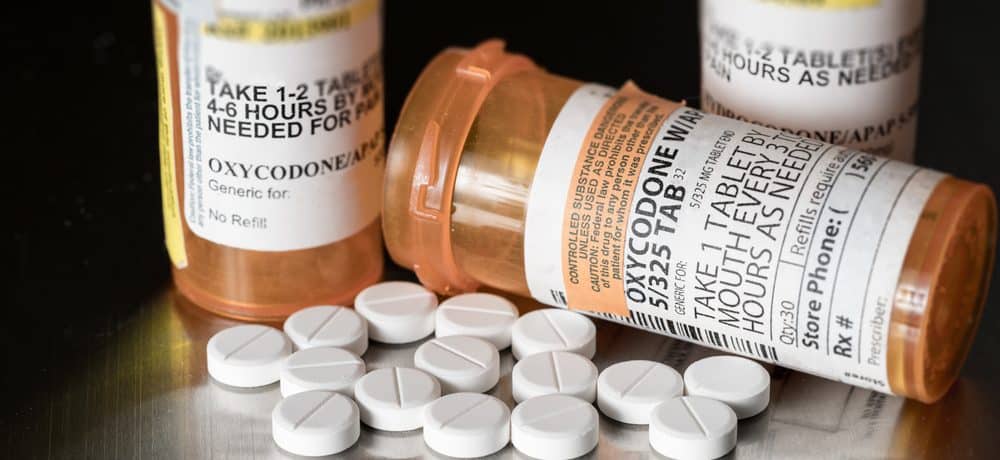
What Is Oxycodone?
Oxycodone is a prescription drug that can be given for moderate to severe pain, and there are dozens of different variations of the drug. It is a potent opioid, meaning that a person can quickly build a tolerance to it, even when they take it exactly as prescribed by their doctor.
Oxycodone is often prescribed even in situations where it shouldn’t necessarily be, such as following dental procedures where a less potent and addictive pain medication could be used instead. However, in the face of the opioid epidemic plaguing the U.S., many doctors are being advised to rethink how and to who they prescribe these medications.
What Is Fentanyl?
Fentanyl is a highly powerful opioid painkiller that is estimated to be up to 100 times stronger thanmorphine.
Like oxycodone, it acts on opioid receptors, but in a much more potent and swift way.
There are some differences that highlight why fentanyl and oxycodone are not the same, despite the fact they’re both opioids.
The first is the strength of fentanyl. While oxycodone is also strong, fentanyl is one of the strongest opioids available, and even a tiny amount can lead to anoverdosein people who are not opioid resistant. There are more restrictions surrounding who should be prescribed fentanyl, and it’s not intended for managing short-term pain. Instead, fentanyl is most often intended for people experiencing severe breakthrough pain on a chronic basis, such as with cancer. It’s also prescribed to people who already receive around-the-clock opioid pain medications.
Respiratory Depression
Both fentanyl and oxycodone can lead tooverdosein the same way. However, it would take significantly less fentanyl for a person to overdose than oxycodone.
The reason these drugs lead to so many overdoses, including many that are fatal, is because they depress the respiratory system. They slow down essential functions including breathing, which is what causes an overdose. The key difference is the potency of fentanyl.
To conclude, are fentanyl and oxycodone the same?
They are the same in that they are both opioids that can be prescribed for pain, they both have the potential for abuse, and they both can lead to serious consequences like respiratory depression. Fentanyl and oxycodone are different in their potency, and also in who they’re intended to be used for in a medical setting. For example, fentanyl is not meant for the treatment of short-term pain outside of a hospital setting.













