Heroin withdrawal is a necessary undertaking when addressing heroin addiction. However, there are options available to detox in a safe and comfortable way.
To recover from heroin addiction, one must first go through the process of ridding the body of heroin and its toxic metabolites. The process is known as detoxification or, more commonly, “detox.” As the body clears the heroin out, the unpleasant experience of drug withdrawal occurs.
For many people with addictions, the fear of withdrawal is a major barrier to escaping their addiction. For some people, that fear keeps them from even trying addiction treatment. However, millions of people have successfully found health and happiness in long-term recovery.
Fortunately, withdrawal and detox don’t have to be a terrible experience. By participating in an inpatient detox and withdrawal program, people can get through the experience safely and comfortably.
Article at a Glance:
- After initially stopping heroin, terrible flu-like symptoms are common, such as runny nose and muscle aches.
- The symptoms of withdrawal from heroin typically start within the first four to 24 hours and peak within 36 to 72 hours.
- Heroin withdrawal symptoms can last for seven to 10 days.
- It is not recommended to quit heroin “cold turkey” or detox at home because many home remedies for heroin detox are unsafe, untested, and unproven.
- A medical facility is the safest and most effective place to detox.
Heroin Withdrawal
Recovery from heroin use is associated with great improvements in health and quality of life. However, the initial cessation of heroin use is associated with a short period of terrible, flu-like withdrawal symptoms as the body rebounds from heroin use. Detoxification involves using medications, counseling and supportive measures to help the individual withdraw safely with minimal symptoms.

Heroin withdrawal symptoms are described as a severe case of the flu, and typically include:
- Mood changes, like agitation and anxiety
- Increased body secretions (runny nose, teary eyes, and sweaty skin)
- Stomach problems (nausea, vomiting, cramping, diarrhea, and loss of appetite)
- Muscle problems (aches, twitching, shivering)
- Sneezing
- Goosebumps
- Yawning
Withdrawal symptoms begin between 4 and 24 hours after the last dose of heroin. The severity and duration of withdrawal may depend on how long the individual used heroin, as well as the amount and method of heroin use.
How Long Does Heroin Withdrawal Last?
Different opioid drugs have different timelines for withdrawal, and it depends on how much and for how long the individual used heroin.
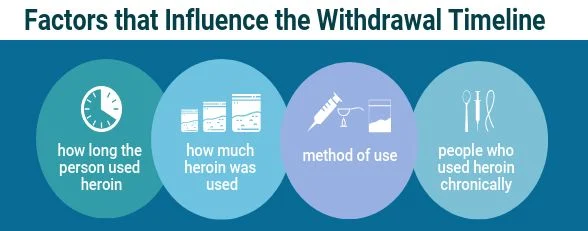
For heroin, the withdrawal symptoms start within the first 24 hours (sometimes as soon as four hours) from the last use, peak within 36 to 72 hours, and last seven to 10 days for most people. People who use heroin chronically may experience some withdrawal for up to three or four weeks.
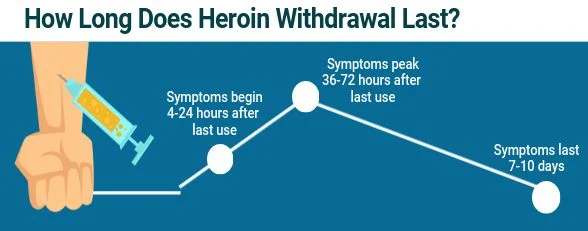
When Does Heroin Withdrawal Start?
For heroin, the withdrawal symptoms start within the first 24 hours (sometimes as soon as four hours) from the last use, peak within 36 to 72 hours, and last seven to 10 days for most people. The severity and duration of withdrawal may depend on how long the individual used heroin, as well as the amount and method of heroin use. People who use heroin chronically may experience some withdrawal for up to three or four weeks. While withdrawal is a necessary undertaking when addressing heroin addiction, there are options available to detox in a safe and comfortable way.
How Long Does Heroin Stay in Your System?
When heroin enters the body, it is rapidly metabolized. This happens so quickly that most of the drug is out of the system within 30 minutes. The half-life of heroin is about three minutes. For example, if someone injects 20 mg of heroin, then 10 mg is left after three minutes, 5 mg after six minutes, etc. Heroin will be completely clear from the body in about 15 minutes for many people, but some people metabolize heroin more slowly. In this case, heroin can stay in the system for 30 minutes or longer. Drug tests can measure heroin in saliva, blood, urine, and hair for different lengths of time.
How Do You Taper Off of Heroin?
A tapering regimen is all about lessening tolerance and dependence over time. Taking less and less of the drug allows the body and nervous system to self-correct and, ultimately, heal itself. By keeping withdrawal symptoms at bay, it is more likely that an individual will continue the recovery process. This is one of the primary reasons replacement therapy is used as well. A person’s environment will play a vital role in deciding how to taper off heroin.
Is Quitting Heroin Cold Turkey a Good Idea?
Quitting cold-turkey is not recommended as it is the most difficult and dangerous way to attempt to address addiction. Medically-supervised detox with withdrawal medications, counseling support, and symptom management make the experience much easier, safer and more likely to result in a successful recovery.

Stopping heroin “cold-turkey” brings about a rapid onset of withdrawal symptoms, which are very difficult to endure. The risk of experiencing a setback during withdrawal is high as the craving to use and stop the symptoms can be overwhelming. When people try to self-taper their heroin use on their own they are seldom successful. A relapse during withdrawal sometimes leads to overdose.
Heroin Withdrawal Medications
Opioid replacement therapy involves a long-acting opioid medication that is used to keep drug cravings and withdrawal symptoms to a minimum without causing a high. Over time, the dose of these drugs can be tapered in a slow and controlled manner until the patient is opioid-free.
Only two opioids are FDA-approved for the treatment of heroin withdrawal: methadone and buprenorphine. Buprenorphine generally has a more favorable side-effect profile than methadone. One type of buprenorphine product used during opioid detox is Suboxone, which also contains naloxone, which blocks opioid receptor sites to prevent any attempts at abuse.
Other medications may also be used during heroin detox to help with specific symptoms. These include sedatives (such as benzodiazepines) and the medication clonidine, which helps reduce some withdrawal symptoms.
About half of people with addictions also suffer from mental health disorders, such as depression or anxiety. Recognizing and treating underlying mental health disorders provides the best success rates for recovery and is an important part of returning the person to good health and functioning.
Heroin Withdrawal Deaths
Withdrawing from heroin is typically safer than withdrawing from alcohol, but it is occasionally fatal. When people die from heroin withdrawal, it’s usually due to excessive vomiting and diarrhea. Untreated, these symptoms can rapidly dehydrate the body and cause dangerously high levels of sodium to accumulate in the blood (hypernatremia) and the heart can fail. Such cases occur when people withdraw from heroin on their own, usually in jail. Such deaths can be prevented by medical supervision in a professional detox facility.
Heroin Withdrawal Tips
The primary tip for heroin withdrawal is not to do it alone. Withdrawal is a difficult experience and willpower alone is seldom adequate to prevent relapse. There is plenty of help out there to make detox and withdrawal safe and less uncomfortable. Utilizing the supports in place is the best way to get on track for long-term recovery. A specialized treatment facility with medically-assisted detox is the safest method for quitting heroin and avoiding relapse.
Heroin Detox
Professional heroin detox is medically-supervised withdrawal from heroin. Detox must be done as part of an overall plan for recovery, which involves much more than simply stopping using the drug. The underlying causes of the addiction and the mental devastation from the addiction itself must be addressed for the best chance of successful recovery and a return to good health and happiness. Detox for a serious addiction like heroin is almost always an inpatient process.
For some people, likely for those whose heroin use was limited, outpatient detox therapy may be an option. Even though their use of heroin was not severe enough to warrant inpatient treatment, they are still psychologically susceptible to using it again. As such, they will be required to attend meetings and counseling sessions.
An inpatient heroin detox program is a natural transition to counseling, which forms a crucial part of the overall treatment plan. A recent study showed that inpatient detox is the most effective way to ensure a successful recovery after discharge.
Other Methods for Detox
Outpatient detox is for patients who have not been addicted to heroin for very long or who abused it in small amounts. To be eligible, their home environment and living situation must be stable and supportive. Regular visits to the treatment center (for medication replenishment, counseling, observation, and tests) will be required.
Various home remedies are advertised, promising to help with heroin withdrawal and detox, but caution is advised. Many remedies are unproven and untested and do not work as well as medically-supervised withdrawal treatment. It is best to speak with a healthcare professional before taking any such medicines.
Some over-the-counter medications can help with withdrawal symptoms, such as acetaminophen for muscle aches, and antidiarrheals and anti-nauseants to help with stomach symptoms.
Acute detoxification is defined as a form of treatment where a patient weans off the abused drug under a doctor’s supervision. The patient will have to be in inpatient status in order for this to happen. By definition, a stay of more than two consecutive days would qualify for “inpatient” status, a threshold that becomes very important when health insurance is factored into the cost of treatment.
One reason for a doctor’s supervision during acute detox is that he may see fit to prescribe medication to help the patient through the detox process. Drugs like Suboxone, while effective at weaning a patient off heroin, can be addictive in their own right; a patient trying to self-medicate while in a susceptible state is not in a position to judiciously administer even beneficial drugs. A doctor, on the other hand, has the benefit of experience and clarity with which to choose medications that can help the patient through detox, and the knowledge of when to taper off those medications, to prevent the patient from developing an addiction to the detox drugs.
Acute Detox Medications
Some of the most commonly used drugs to help addicts through heroin detox include:
- Methadone
- Buprenorphine
- Phenobarbital
- Chlordiazepoxide (Librium)
- Diazepam (Valium)
- Lorazepam (Ativan)
- Oxazepam (Serax)
Drugs like chlordiazepoxide and diazepam are anti-anxiety medications, which are useful for keeping patients calm and relaxed during the process.
Symptoms of Acute Detox
For patients whose heroin abuse has been chronic or extreme, the services offered by an acute detox program could be the difference between life and death. One of the symptoms of withdrawal from heroin, or other similar opioids, is the user experiencing suicidal thoughts or ideas. The National Institute on Drug Abuse explains that suicidal ideation may be found in opioid abusers even without withdrawal. Major depression also accompanies withdrawal, so it is vital that the patient not be left alone at a time when the patient is going through very difficult periods of mental and physical distress. Acute heroin detox programs provide counselors and therapists on hand, who can offer precise support and encouragement to addicts who are struggling with the transition.
A controversial method of detox, known as “rapid detoxification,” is carried out while patients are under general anesthesia. Patients effectively “sleep through their withdrawal.” Doctors give the patients injections of medications known as opiate blockers, which put a hard stop on the effects of the heroin in their system, while also administering other drugs, like anti-anxiety medications or muscle relaxants, to help with the withdrawal. This causes rapid withdrawal from the physical effects of heroin. From start to finish, the process can last from 4-8 hours; discharge from the program can be completed 48 hours after recovery from the anesthesia.
Rapid detoxification is a dangerous method, so it is only used for patients who are at risk for their withdrawal symptoms endangering their lives. It may also be employed for patients who do not respond to conventional detox programs.
Ultra-Rapid Detoxification
The ultra-rapid detoxification can is a complete detox in under an hour, but it is very dangerous. The National Institute on Drug Abuse reported on a study from 2006 that found “three serious adverse events” from a patient population of 35. The study concluded that using general anesthesia to sedate patients during withdrawal provided no benefit to treatment, specifically saying that no evidence was found to support claims that rapid detoxification was a “fast and painless method” by which a heroin addiction could be controlled.
Outpatient detox is for patients who have not been addicted to heroin for very long or who abused it in small amounts. For such users, they are likely to have withdrawal symptoms that range from the mild to moderate, enough that they can merely collect their medication from a treatment center and go home.
This offers patients the comfort of enduring the still-uncomfortable symptoms of withdrawal privately if a doctor feels they can do so safely. There is little chance of an impulsive relapse, meaning that the patient’s environment and home situation need to pass an assessment before outpatient detox can be approved. Day-to-day activities, such as school and work, can continue with minimal interruption, opposed to acute detox.
The freedom of an outpatient detox program comes with the responsibility of the patient having a large stake in his own recovery. The Fix explains that visits to the treatment center (for medication replenishment, observation, and tests) have to be regular; for that reason, the visits themselves can be quite lengthy, lasting hours at a time.
Helping Someone Withdrawing or Detoxing From Heroin
It’s best to talk to an addiction specialist team to obtain advice before helping a loved one through the detox and withdrawal process. Addiction specialists are trained in how to work with people in withdrawal. They can offer expert support with the task of helping a loved one through the withdrawal process. To talk to a specialist, call us, or sign up for online counseling services through The Recovery Village Telethealth App.
Before withdrawal and detox begin, it’s important to clear all drugs and drug paraphernalia out of the house to avoid tempting the individual.
It can be very stressful to watch someone go through heroin withdrawal. Although heroin withdrawal is seldom deadly, stopping heroin can lead to very uncomfortable symptoms within only a few hours. Besides the physical symptoms, the person withdrawing may show psychological symptoms, such as confusion, anxiety, and aggression.
Because recovery is a lifelong process, the individual will require ongoing support. The person in recovery will need a strong support system after detox completes. This support system may include long-term professional counseling sessions. Some counseling sessions may be available to friends and family as well.
Therapy After Detox
Regardless of the merits of acute heroin detox versus outpatient heroin detox, neither approach will be very successful without the presence of counseling following the actual detox process. As mentioned earlier, a heroin addiction devastates both the mind and the body. Detox addresses the damage done to the body; counseling addresses the mind.
For an addict in an outpatient detox program, one of the conditions of the freedom of movement is that they have to attend regular counseling sessions. Even though the abuse of heroin was not severe enough to warrant acute treatment, the initial use of heroin suggests that they are still psychologically susceptible to using again. Patients in an outpatient program will learn much the same thing from therapy, which is why it is imperative that everyone who goes through any kind of detox follows it up with counseling. Any detox program, inpatient or outpatient, is incomplete without counseling.
A user going through an inpatient heroin detox program will have a natural transition to counseling, which would be made part of the overall treatment plan. The patient’s acute status implies that they are in great need of therapy, as the heroin would have had to have wreaked a considerable amount of damage for the user to need multiple consecutive days of treatment. In therapy, the patient will gain a deep understanding of the reasons the user turned to heroin, and how they can apply that understanding to learn how to say no, think positively and live clean.
The point is echoed by an August 2014 study published in the Journal of the American Medical Association. Researchers found that opioid-dependent patients who were hospitalized did not use drugs in the first month after they were discharged; similarly, patients in an outpatient treatment group used drugs less than they did before, for up to six months following the conclusion of their treatment. The study concluded that treatment for heroin addiction was most effective if it incorporated both acute and outpatient treatment.
Finding a Heroin Withdrawal & Detox Center
The do-it-yourself detox methods are not worth the risks and can lead to far more damaging effects on the body. Undergoing detox at a professional facility is a safe and effective way to rid the body of drugs like heroin.


British Journal of Clinical Pharmacology. “Pharmacological strategies for detoxification.” February 2014. Accessed May 9, 2019.
Industrial Psychiatry Journal. “Newer approaches to opioid detoxification.” December 2012. Accessed May 9, 2019.
Journal of Addiction. “Predictors of relapse after inpatient op[…]ng 1-year follow-up.” August 24, 2016. Accessed May 9, 2019.
Journal of Addiction Medicine. “A systematic review on the use of psycho[…] of opioid addiction.” March 2016. Accessed May 9, 2019.
Journal of the American Medical Association. “Buprenorphine treatment for hospitalized[…]mized clinical trial.” August 2014. Accessed May 9, 2019.
Journal of the Society for the Study of Addiction. “Yes, people can die from opiate withdrawal.” February 2017. Accessed Amy 9, 2019.
Liebschutz JM, Crooks D, Herman D, et al. “Buprenorphine Treatment for Hospitalized[…]ized Clinical Trial.” JAMA Intern Med. 2014. Accessed September 20, 2021.
NIDA. “Study Finds Withdrawal No Easier With Ultrarapid Opiate Detox.” National Institute on Drug Abuse, October 1, 2006. Accessed September 20, 2021.
NIDA. “Thoughts of Suicide May Persist Among Nonmedical Prescription Opiate Users.” National Institute on Drug Abuse, March 4, 2013. Accessed September 20, 2021.
U.S. National Institute on Drug Abuse. “Comorbidity: Substance use disorders and[…]her mental illnesses.” August 2018. Accessed May 9, 2019.
U.S. Pharmacist. “Acute opioid withdrawal: Identification […]treatment strategies.” November 17, 2016. Accessed May 9, 2019.
The Recovery Village aims to improve the quality of life for people struggling with substance use or mental health disorder with fact-based content about the nature of behavioral health conditions, treatment options and their related outcomes. We publish material that is researched, cited, edited and reviewed by licensed medical professionals. The information we provide is not intended to be a substitute for professional medical advice, diagnosis or treatment. It should not be used in place of the advice of your physician or other qualified healthcare providers.